AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Define dendrite cell12/19/2023  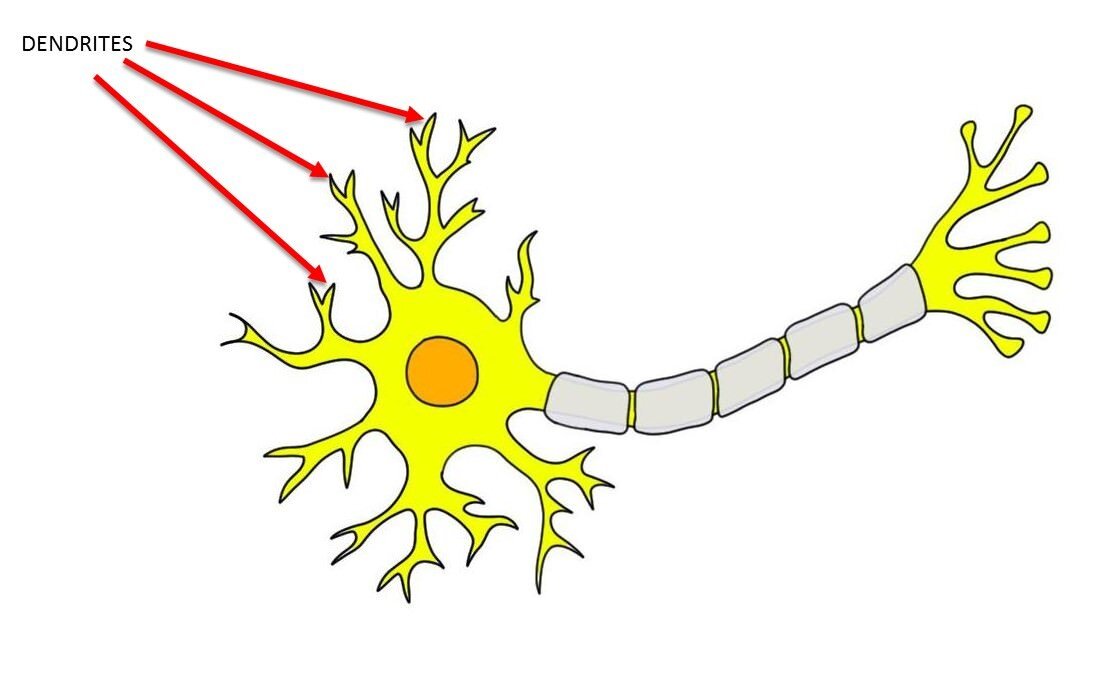
The healthy controls were asymptomatic healthy individuals with a clear healthy cornea without vital staining and normal tear function tests. The aqueous-deficient DED group was further stratified into two subgroups, the immunologic subgroup (including cases with Sjögren's syndrome, as defined by American–European consensus group criteria, 28 and graft versus host disease ) and the nonimmunologic subgroup. In the presence of a low Schirmer's test result (≤5 mm) and a low TBUT (<10 seconds), the patient was categorized as aqueous-deficient DED. The patients were categorized to have evaporative DED if they had TBUT less than 10 seconds and Schirmer's test results greater than 5 mm. 24 – 27Īll these patients had typical symptoms of DED for a duration of 6 months or more. 22, 23 Thus, recent studies have assessed DC morphology in their evaluation of IVCM changes of the cornea in conditions other than DED. Further, while previous studies have revealed changes in DC density, morphologic changes of DC have recently gained attention, as increased size of DCs is a sign of their maturation, activation, MHC-II (HLA-DR) expression, and their antigen presentation capability. 17 – 21 However, the extent of DC changes remain unclear in different subtypes of DED. 15, 16 Using IVCM in patients with DED, recent studies have shown changes in DCs in the corneal subbasal layer. 11 – 14 With IVCM, all cellular structures, including epithelial DCs in the cornea, can be clearly visualized, and have been shown to be consistent with immunohistochemistry findings. In vivo confocal microscopy is a noninvasive imaging modality that enables studying the cornea at a cellular level. To evaluate changes in DCs in patients with DED, corneal in vivo confocal microscopy (IVCM) has lately been used. These changes, which reflect the degree of immune activation and inflammation in DED, can be used for clinical practice and endpoints in clinical trials. 
When aqueous-deficient DED with underlying systemic immune disease (Sjögren's syndrome and graft versus host disease) were compared with nonimmune conditions, the immunologic subgroup showed significantly higher DC density, DC size, and number of dendrites (all P < 0.05).Ĭorneal IVCM demonstrated differential changes in DC density and morphologic DC parameters between subtypes of DED. However, there were no significant differences in morphologic parameters between DED subtypes. Comparison between aqueous-deficient and evaporative subtypes demonstrated that DC density was significantly higher in aqueous-deficient subtype (189.8 ± 36.9 vs. 
These DC parameters were compared among all dry eye and control groups.Ĭompared with the controls, patients with DED had significantly higher DC density, larger DC size, higher number of dendrites, and larger DC field (all P < 0.001). 
For all subjects, images of laser scanning in vivo confocal microscopy (IVCM) of the central cornea were analyzed for DC density and DC morphology (DC size, number of dendrites, and DC field). Based on clinical tests, eyes with DED were categorized into two subtypes: aqueous-deficient ( n = 35) and evaporative ( n = 24). This retrospective study included 59 eyes of 37 patients with DED and 40 eyes of 20 age-matched healthy controls. To evaluate density and morphology of corneal epithelial immune dendritic cells (DCs) in different subtypes of dry eye disease (DED) using in vivo confocal microscopy (IVCM). 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
